State of the art
In October 2020, a Dutch research team revealed a correlation between low vitamin K status and more severe COVID-19.1 Published in Clinical Infectious Diseases, their study showed a clear vitamin K deficiency in COVID-19 patients—but only extra-hepatically. The vitamin K-dependent proteins in the liver, involved in blood clotting, were properly activated, while other vitamin K-dependent proteins in the rest of the body were not. These extra-hepatic proteins (that are working outside the liver) play numerous functions: normal coagulation, preventing inflammation, or preventing calcium from depositing in soft tissues, like arteries or the lungs; instead leading it to our bones and teeth for good mineralization.
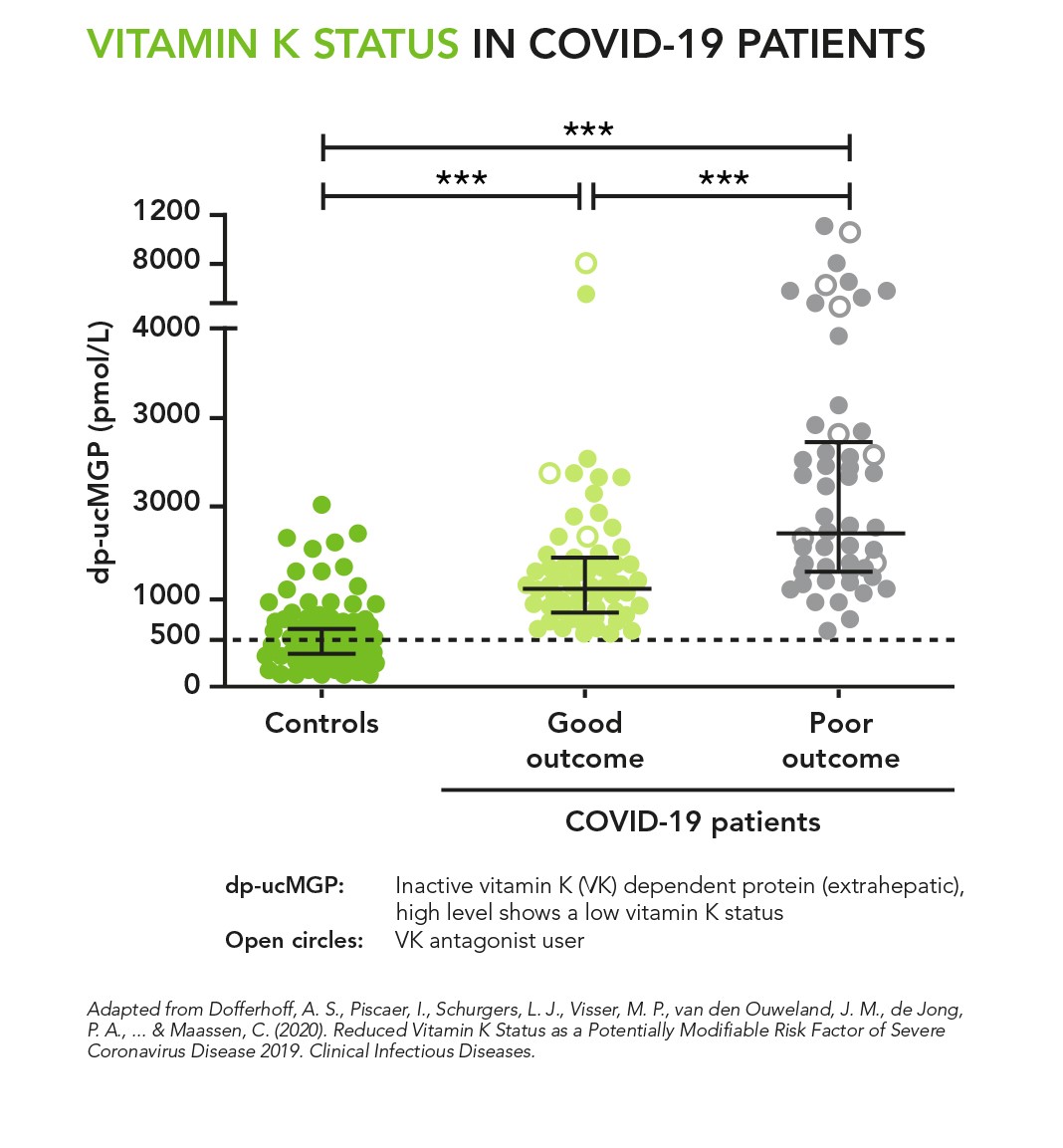
Figure 1: Vitamin K status in COVID-19 patients. High circulating dp-ucMGP levels reflects low extrahepatic vitamin K status.
The authors suggest that an extra-hepatic vitamin K deficiency, like the one found in COVID-19 patients, could lead to an imbalance within the coagulation machinery, and accelerate the elastic fibres degradation in the lungs. For this reason, they explain, in a second article published in the British Journal of Nutrition later in 2020,2 that an impaired vitamin K metabolism is a potential missing link between thromboembolism (the formation of blood clots) and lung damage in COVID-19.

Figure 2: Proposed sequential steps, linking SARS-COV-2 pneumonia to vitamin K insufficiency, pulmonary damage and thrombogenicity.
Intrigued, a second research team in Denmark performed similar research to observe whether vitamin K status could predict COVID-19 outcomes. Their study, published in Nutrients 9 June 2021, confirmed that lower vitamin K status correlates with worse COVID-19.3
“Our study shows that low vitamin K status predicts mortality in patients with COVID-19. Randomized, double-blind placebo-controlled clinical trials are now needed to document potential beneficial effects of vitamin K2 supplementation on the course of COVID-19,” says Allan Linneberg, MD, PhD, Director of Center for Clinical Research and Prevention Bispebjerg and Frederiksberg Hospital (Denmark), and lead author of the study.

Figure 3: Kaplan-Meier plot of 30-days cumulated risk of dying, stratified by levels of vitamin K status. Lower dephosphorylated uncarboxylated matrix Gla protein (dp-uc-MGP) level reflects higher vitamin K status.
How to explain such results?
The Dutch research team, in its review, made one hypothesis: the triage theory. This theory implies that, in times of scarcity, the body preserves its most vital functions, at the expense of other, less crucial ones. Since normal blood clotting is one of the most important functions, the authors explain that the body would save its vitamin K stores specifically for the activation of the crucial coagulation factors—most of them located in the liver. For that reason, if the body’s supply in vitamin K is insufficient, there is not enough left to activate all other K-dependent proteins.
“Considering that vitamin K is important for regulating lung health and blood clotting, vitamin K deficiency during COVID-19 may make both those problems worse,” explains Jona Walk, MD, PhD and Resident in Internal Medicine at the Canisius Wilhelmina Hospital, Nijmegen, The Netherlands.
Could vitamin K supplementation help?
On the contrary to vitamin K1, K2 is directly distributed extra-hepatically, and could therefore play an important role to restore this recently discovered imbalance.
Because of their structural differences, vitamins K1 and K2 do not have the same biological activities. With K2, the role of vitamin K extends beyond blood clotting, as it also regulates other important metabolic processes, such as calcification and inflammation. K1 is easily found in a balanced diet, which is not the case for K2. Deficiency might be more common than commonly considered.
Kappa Bioscience was contacted by both research teams, and accepted their offers to provide financial support, as well as to supply K2VITAL® (all-trans vitamin K2 MK-7), for intervention trials.
Next steps…
Researchers now wonder whether supplementation with vitamin K2 might help. Canisius Wilhelmina Hospital has initiated the first ever clinical trial to explore whether supplementation with vitamin K could benefit COVID-19 patients.
The prospective, randomized, double-blind, placebo controlled “KOVIT” clinical trial aims to evaluate whether vitamin K status affects coagulopathy, and elastic fibres degradation in the lungs. In total, 40 COVID-19 patients, hospitalized with respiratory failure, will be included and given 999 micrograms of vitamin K2 MK-7, or placebo, for 14 days.4
…and synergies
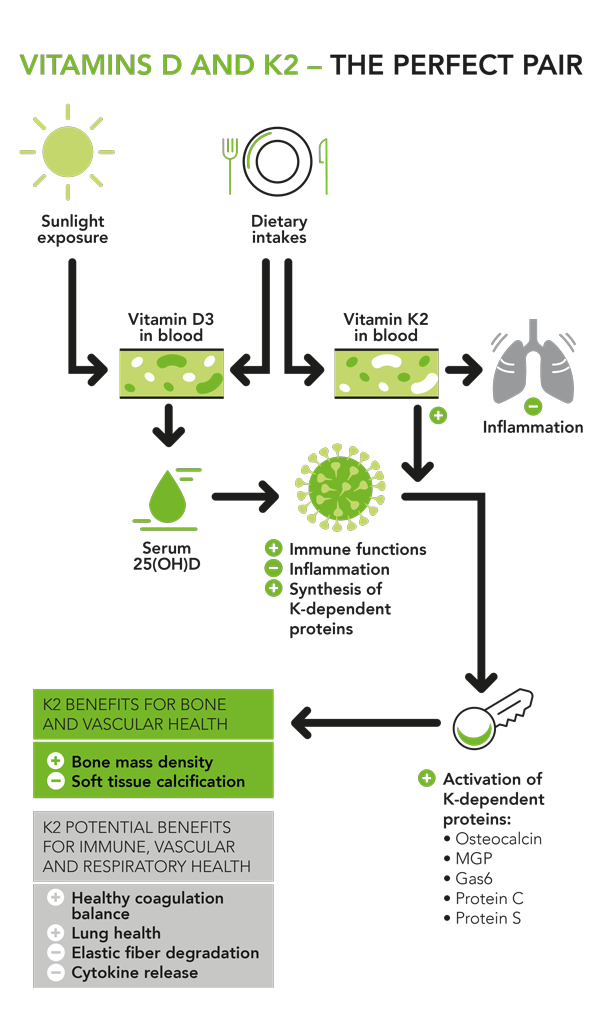
In addition, it is important to understand that vitamins D and K2 work together to properly regulate calcium metabolism. What is the link between calcium and immunity? Higher vitamin D levels imply an increased absorption of calcium. This precious mineral plays key roles, but requires vitamin K2 for a good regulation. K2 prevents calcium from being deposited in soft tissues, like arteries or lungs, and leads it where it is really needed: to the bones. High supplementation with D3 alone could therefore be detrimental for people who are also deficient in K2, scientists say.5
|
|
|
References
1 Dofferhoff, A. S., Piscaer, I., Schurgers, L. ., Visser, M. P. J., van den Ouweland, J. M., de Jong, P. A., ... & Janssen, R. (2020). Reduced Vitamin K Status as a Potentially Modifiable Risk Factor of Severe Coronavirus Disease 2019. Clinical Infectious Diseases.
2 Janssen, R., Visser, M. P., Dofferhoff, A. S., Vermeer, C., Janssens, W., & Walk, J. (2020). Vitamin K metabolism as the potential missing link between lung damage and thromboembolism in Coronavirus disease 2019. British Journal of Nutrition, 1-8.
3 Linneberg, A.; Kampmann, F.B.; Israelsen, S.B.; Andersen, L.R.; Jørgensen, H.L.; Sandholt, H.; Jørgensen, N.R.; Thysen, S.M.; Benfield, T. The Association of Low Vitamin K Status with Mortality in a Cohort of 138 Hospitalized Patients with COVID-19. Nutrients, 2021, 13, 1985.
4 https://www.clinicaltrials.gov/ct2/show/NCT04770740
5 Walk, J., Dofferhoff, A. S., van den Ouweland, J. M., van Daal, H., & Janssen, R. (2020). Vitamin D-contrary to vitamin K-does not associate with clinical outcome in hospitalized COVID-19 patients. medRxiv.

